Mycosis or fungal infection of the foot is a pathology that occurs in 40% of people. The reasons for the development of infection can be many: from violation of hygiene rules to the development of serious diseases of internal organs and systems. Toenail fungus can be cured using medications and folk methods, but only with preliminary diagnosis and consultation with a dermatologist.
How to Identify Foot Fungus
With the development of foot fungus, damage to the dermal tissue occurs. The first signs of the disease do not have a pronounced intensity, so they are often perceived as normal roughness and irritation of the skin of the legs.
Despite the prevalence of the pathology, few people know how to recognize foot fungus. Foot fungus appears 3 to 5 days after infection. The longer the fungus progresses, the more pronounced its symptoms will be.
Symptoms of a fungal infection of the skin of the feet:
- at the earliest stage, the patient notices severe peeling of the skin, which, even after standard treatment of the feet and the use of creams, is not completely eliminated;
- itching gradually begins to bother you, which intensifies every day and causes severe discomfort;
- Along with itching, a sour smell appears, which appears when a fungus develops on the skin, it is accompanied by a strong smell of sweat (due to dysfunction of the subcutaneous glands, sweating increases);
- There is also a change in the shade of the skin of the foot, the epithelium acquires an unnatural color at the site of the lesion: bluish, greenish or even gray-black (in advanced cases).
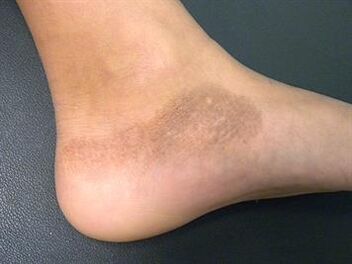
With foot fungus, onychomycosis (fungal infection of the nail plates) often occurs, so the patient's nails may begin to break, deteriorate and change color. In rare cases, general health deteriorates (temperature rises, constant weakness and apathy bother you).
Important!It is impossible to independently determine the stage and type of fungus. Therefore, if you suffer from any dermatological disease, you should consult an experienced specialist.
Why are foot fungus dangerous?
Many people suffering from foot fungus do not take it seriously, believing that the disease will go away by itself, or until it causes unbearable pain, they do not seek to get rid of the infection.
Note!The peculiarity of foot fungus is that the fungal infection is contagious, and since a person often walks without shoes, the patient exposes a large number of people to the risk of infection.
Foot fungus does not cause life-threatening complications, however, if the disease is left untreated, complications may occur:
- transition of the disease to a chronic form;
- weakened immunity;
- increased risk of developing other skin pathologies.
Dermatologic complications include:
- allergy;
- focal or regional spread of the rash;
- widespread skin lesions;
- papule formation, erythema, eczema.
Complications occur in patients who neglect treatment for foot fungus. If treatment is started on time, the disease is eliminated without consequences.
What causes foot fungus?
Foot fungus is caused by an infection. Fungal spores have the ability to maintain vital activity even in the absence of contact with the skin.
Before answering the causes of foot fungus, it should be noted that experts identify several groups of people susceptible to fungal infections.
- with weakened immunity;
- with vascular diseases;
- violate hygiene rules.
In case of foot fungus, the most common causes of infection are:
- diseases associated with immunodeficiency;
- rarely change socks, wear poor quality shoes;
- visiting public baths (without respecting personal hygiene);
- nail fungus;
- increased sweating of the feet.
One of the factors contributing to the development of foot fungus is the psychosomatic nature of the disease. Experts confirm that a violation of the psycho-emotional state greatly affects the immune system, weakening it. A weak immune system is not able to resist the fungus, which increases the risk of developing mycosis.
Is foot fungus contagious?
Specialists in the dermatological medical field have proven that foot fungus is a disease that occurs after contact of the skin of the feet with fungal spores.
The peculiarity of this type of infection is the long-term survival of spores falling on any surface. Additionally, even on the skin of the foot, fungal spores can remain dormant for many years, and when favorable conditions arise, they can be activated.
It is the ability to maintain infectious activity in the spore state for many years that presents the greatest danger. It is impossible to completely prevent infection. The fungus thrives in a humid environment, so compliance with hygiene standards is the most effective way to prevent infection.
Important!Given the way foot fungus is transmitted, it is also important to consider the risk of infection for people in contact with the patient, particularly those who live with them.
How is foot fungus transmitted?
The fungal infection is transmitted through household contact. The main method of infection is when the spores get on the healthy skin of the feet.

How is foot fungus transmitted? There are two types of fungal foot infection.
- Direct: contact of the foot with an infected surface, contact with the feet of a patient, contact with an animal whose coat contains spores.
- Indirect: contact with personal effects of a patient with mycosis (socks, shoes, towel, etc. ), contact with care items for an infected animal.
In 60% of cases, infection occurs when visiting public places (saunas, baths, beaches, etc. ). There is also danger during a pedicure procedure if items used in the salon are not handled correctly.
Types of foot fungus
Depending on how the foot fungus is transmitted (the area to which the spores attach), different forms of infection can develop.
Dermatologists identify the main forms of foot fungus, which differ in the location of the affected area.
- Interdigital. Mycosis affects the skin between the toes. With this form, we distinguish two stages: intertriginous and squamous. Most often, the infection becomes chronic, because the area between the fingers provides the most favorable conditions for the proliferation of fungal spores.
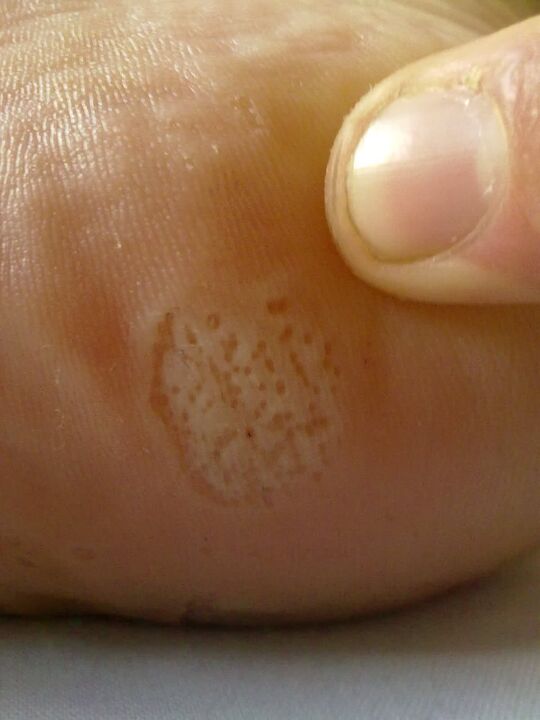
- Plantar. The epithelial layers of the sole of the foot are affected by mycosis. A characteristic sign is severe keratinization, cracking and peeling of tissues.
- Dyshidrotic. The most painful form of fungus on the feet, accompanied by the formation of vesicles and bubbles on the sole of the foot, which, when bursting, lead to secondary infection.
- Deep mycosis. In case of deep mycosis, a large part of the foot is affected and the infection penetrates deep into the skin.
- Onychomycosis. This form can be the cause or consequence of a fungal disease of the skin of the legs. With onychomycosis, the toenail plates become infected.
The most common form of pathology is interdigital. However, deep and dyshidrotic mycoses, which are difficult to completely cure, are considered dangerous.
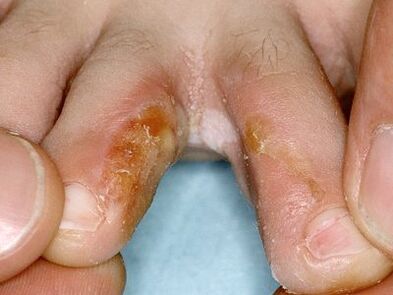
Internumeric form
With interdigital fungus, symptoms appear after 2 to 3 days. Subsequently, the signs of infection become more and more pronounced. It is almost impossible to identify foot fungus on your own at the initial stage. The signs of the disease are similar to insufficient hydration of the feet.
Note!In case of infectious lesions of the feet, interdigital fungus of children's feet is diagnosed in 70% of cases. Children move around a lot, often spend time outside and are often without shoes or socks.
Since the signs of the disease in the first days are not characteristic, how can you tell if there is a fungus? In traditional medicine, there is a special method that allows you to identify the infection at the initial stage: immerse your feet in a solution of manganese and wait 20 minutes.
If after the procedure the color of the entire skin has changed, but the areas between the fingers remain the same shade, most likely there are pathogenic microorganisms on the dermis.
Stages and their manifestations
Interdigital mycosis progresses in three stages. Each has manifestation characteristics. The more the infection progresses, the more obvious the signs become. Gradually, the disease brings not only discomfort, but also painful torment.
initial stage
At the initial stage, the patient begins to be bothered by peeling of the skin of the legs in the space between the toes. The plantar area of tissues from the little finger to the third finger is most affected.
How does the squamous-hyperkeratotic stage manifest?
In the squamous-hyperkeratotic stage, the processes of keratinization and desquamation of the affected epithelial particles begin on the surface of the foot. The skin around the localization sites becomes red, the burning sensation and the feeling of constant itching intensify.
In the intertriginous stage, swelling between the fingers is noticeable, erosion occurs in keratinized areas, and suppuration may begin. The symptoms of the previous stage intensify.
Dyshidrotic stage

In the dyshidrotic stage, blisters form, the area of the lesion increases, spreading further along the foot. Fungal infection also affects the nails.
Interdigital fungus on the feet should not be allowed to develop; treatment should be initiated at the first suspicion. In this way, serious complications leading to the risk of developing purulent infections can be avoided.
How to treat foot fungus
A dermatologist will tell you how to eliminate foot fungus. Treatment of the disease can have many nuances, since there are many types of fungal infections. The specialist prescribes diagnostics and individually determines what the nail fungus found in the patient is afraid of.
For fungal foot infections, two methods are used:
- medicinal;
- popular
Drug therapy is the main one. Home treatment with folk remedies is an additional effect on the pathological process, eliminating the symptoms.
Treatment for mycosis can last several months. It will not be possible to eliminate the disease in a few weeks.
Medicinal method
When choosing antifungal drugs, you should not only think about how to quickly cure foot fungus. Some drugs can only eliminate the signs of the disease without destroying the spores located deep under the layers of the epithelium. An incompletely treated mycosis can quickly cause a relapse.
Ointments
You can treat toenail fungus at home using topical products. Ointments are effective at the initial stage of the disease, and in advanced forms they are used in combination with tablets.
Dermatologists recommend ointments containing disinfectant, anti-infectious and regenerating substances against foot fungus.
Symptoms and treatment of fungal infection are interrelated, since the use of antifungal ointments is aimed at eliminating signs of pathology and jointly providing an antifungal effect.
Important!The effectiveness of the topical agent is noted at the first stage of treatment, however, in case of significant lesions of the feet, the use of ointments alone may not be enough.
Pills
Systemic antifungal drugs have a general effect. The dosage of the active substance in tablets is usually much higher than in ointments. The advantage of the tablet form of the drug is that the drug has a stronger effect and not only eliminates the infection, but also prevents relapses.
If you treat foot fungus at home, you can take pills, but the drugs have contraindications, so taking them is allowed only in consultation with your doctor.
Important!Tablets are contraindicated in childhood, breastfeeding and during pregnancy.
Antifungal drugs rarely cause side effects, have minimal contraindications and allow you to defeat mycosis in the shortest possible time.
Also, to treat fungus, ointments, solutions or sprays are used in combination with taking tablets.
Traditional treatment method
There are many methods for removing foot fungus using folk remedies. Keeping in mind the way of transmission of foot fungus, we can conclude that home therapy methods should be aimed at eliminating the infection from the surface of the foot. Folk remedies also have an antisymptomatic effect.
Note!Treatment with folk remedies does not replace medication. Alternative medicine is only recommended as a complementary therapy.
According to reviews, methods for removing foot fungus will help you achieve maximum efficiency.
Vinegar and hydrogen peroxide
Vinegar and hydrogen peroxide - pharmacy hydrogen peroxide is mixed with alcohol and table vinegar. Everything is in equal proportion. A cotton swab is moistened in the resulting solution and the skin at the site of the foot lesion is generously treated with it. The duration of treatment lasts up to 1 month. The procedure should be carried out daily in the morning and evening.
Celandine juice

Celandine juice - after the preparatory procedures for cleaning the skin of the feet, prepare a solution for the bath. After that, they begin to use celandine juice. Freshly picked, the plant exudes juice from its stem, which eliminates skin infections. Celandine juice is used to treat all affected areas of the foot for a month. The product should be applied 2 times a day.
Soda baths
Soda foot baths have a preventive and therapeutic effect. Place your feet in a container containing two liters of water in which two tablespoons of baking soda are dissolved for a quarter of an hour. Then the feet are not washed, but simply dried with a towel. Baths are carried out for at least two weeks.
How to treat foot fungus using folk remedies or medications is, of course, decided by the patient himself, but it is better to give preference to joint therapy, which will allow you to achieve quick and lasting resultsin the fight against mycoses.
Knowing how foot fungus is transmitted, the patient must understand that treatment of the disease consists above all of prevention. If prevention is not followed, foot fungus can develop again. To prevent relapses, it is necessary to maintain hygiene, strengthen the immune system and follow the dermatologist's recommendations regarding treatment.
















